The glucagon gene is expressed along the GI tract in highly specialized gut endocrine cells, designated L cells. The majority of L cells are classically thought to be located in the distal gut, predominantly the ileum and colon, however small numbers of GLP-1+ L cells can be found throughout the small bowel..
Gut endocrine cells were classically named for the predominant hormone they produced, however it has long been recognized that the majority of enteroendocrine cells are plurihormonal, synthesizing and seceting multiple peptide hormones. Beyond classical concepts encompassing secretion of peptide hormones, gut endocrine cells may also relay information to sensory neurons through mechanisms linking synthesis and release of neurotransmitters in close proximity to sensory neurons expressing cognate neuroreceptors. Bohórquez and colleagues determined that sensory nerve fibers were actually much closer anatomically then blood vessels to murine gut endocrine cells, using PYY+ cells as the enteroendocrine protoype cell. This intimate interaction can be recapitulated using an in vitro co-culture system, whereby enteroendocrine cell respond to the presence of neurons by elongating cytoplasmic processes towards the neuron. Furthermore, a subset of gut endocrine cells exhibit an extremely long residual t1/2 (detected 60 days after labeling) in the gut epithelium in vivo, consistent with a more stable biosensor cellular system. Gene expression profiling of purified CCK+ enteroendocrine cells revealed expression of genes encoding for presynaptic proteins, including synapsin 1, piccolo, bassoon, MUNC13B, RIMS2, latrophilin 1, and transsynaptic neurexin 2. Pyy-GFP enteroendocrine cells also expressed DOPA decarboxylase and tyrosine hydroxylase, essential enzymes in synthesis of the neurotransmitter dopamine and expression of a cohort of postsynaptic genes was also revealed. Using a rabies virus infection model, the authors demonstrated uptake of the virus by enteroendocrine cells, and local proagation of the virus to adjacent sensory neurons, demonstrating that enteroendocrine cells are synaptically connected to efferent neurons in vivo Neuroepithelial circuit formed by innervation of sensory enteroendocrine cells J Clin Invest. 2015 Jan 2. pii: 78361. doi: 10.1172/JCI78361
Habib and colleagues used flow cytometry to isolate different GLP-1-producing "L cells" from various regions of the gut. Analysis of peptide homone gene expression and immunocytochemistry revealed considerable differences in the extent of hormone gene expression in L cells from the upper small bowel versus the colon. Moreover, considerable overlap in gene expression profiles was observed comparing L cells vs. K cells. Indeed, "L cells" from the upper small bowel were more similar to K cells, rather than to colonic L cells. These data provide considerable information about gene expression profiles in L cells and reaffirm the plurihormonal nature of gut endocrine cells. Furthermore, the authors emphasize the considerable similarity of L vs. K cells, despite obvious differences in relative expression of key peptide hormones. Overlap of Endocrine Hormone Expression in the Mouse Intestine Revealed by Transcriptional Profiling and Flow Cytometry Endocrinology. 2012 Jun 8. [Epub ahead of print]
Complementary analyses of uni-vs. plurihormonal enteroendocrine cell populations was reported by Egerod and colleagues. Using a reporter gene expressing GFP under the control of the CCK promoter, numerous GFP+ cells were detected throughout the small and large bowel, that co-expressed secretin, GIP, ghrelin, proglucagon, neurotensin, and PYY. The plurihormonal nature of CCK+ cells was confirmed in endocrine cells isolated from both villous and crypt fractions. Although the results obtained with RNA and immunohistichemical analyses were generally in agreement, ghrelin immunoreactivity was not detected in CCK-eGFP+ cells. Furthermore, the quantity of secretin-derived peptides, assessed by LC-MS, was lower than predicted by relative abundance of secretin mRNA. Coversely, ablation of enteroendocrine cell populations using a proglucagon pomoter-diptheria toxin transgene revealed loss of cells expressing CCK, neurotensin, GIP, and secretin. Immunohistochemical analsis of human gut endocrine populations revealed supportive evidence for the complex plurihormonal nature of enteroendocrine cells. In human, somatostatin or ghrelin was generally not-co-expressed with other peptide hormones in the small bowel. A Major Lineage of Enteroendocrine Cells Coexpress CCK, Secretin, GIP, GLP-1, PYY, and Neurotensin but Not Somatostatin Endocrinology October 12, 2012 en.2012-1595
Two commonly studied enteroendocrine cell lineages include GIP-secreting K cells and GLP-1-secreting L cells. As gut K cells are sparse and difficult to study, there is little known about the molecular biology of the GIP-secreting K cell. Parker and colleagues isolated purified populations of non-immortalized murine K cells from transgenic mice expressing a yellow fluorscent protein under the control of the GIP promoter. Murine K cells were found to express Kir6.2, Sur1, Sglt1, GPR40, GPR119, and GPR120 and GIP secretion was stimulated by glucose, cyclic AMP and linoleic acid as well as tolbutamide but not by modulation of tast receptor activity. GIP+ cells also expressed the proglucagon gene, and at a much higher level, the Pyy gene. See Nutrient-dependent secretion of glucose-dependent insulinotropic polypeptide from primary murine K cells. Diabetologia. 2009 Feb;52(2):289-98.
The origin of L cell or enteroendocrine cell lineages remains a challenging research issue. In an elegant paper Targeted ablation of secretin-producing cells in transgenic mice reveals a common differentiation pathway with multiple enteroendocrine cell lineages in the small intestine. Development. 1999 Sep;126(18):4149-56. Rindi and Leiter addressed this question by ablating cells expressing a secretin-HSVTK transgene with gancylovir. Remarkably, cells expressing CCK, PYY/enteroglucagon as well as secretin were markedly reduced in number. These studies suggest a developmental relationship between these cell types, possibly invoking a multipotential endocrine stem cell precursor that gives rise to multiple lineages.
Terry et al identified a pivotal role for Islet-1 (Isl1) as a key regulator of enteroendocrine cell development. Co-expression of islet-1 and GLP-1, GIP, somatostatin, gastrin and ghrelin was observed in the normal gut. Using the villin-Cre mouse, deletion of isl1 was achieved in the gut epithelium. Isl1 was expressed in 84% of GLP-1-immunopositive cells and 38% of GIP+ cells. Ablation of isl1 in gut endocrine lineages produced profound reductions in the number of GLP-1+ cells and in the expression of proglucagon mRNA transcripts. Furthermore, loss of epithelial isl1 was associated with fat malabsorption while pups were on high fat milk (increased oil red O staining), and impaired oral, but preserved intraperitoneal glucose tolerance in adult mice, with reduced GSIS following oral glucose. See Impaired enteroendocrine development in intestinal-specific Islet1 mouse mutants causes impaired glucose homeostasis Am J Physiol Gastrointest Liver Physiol. 2014 Sep 11:ajpgi.00390.2013
Although the "master regulators" of enteroendocrine cell lineage remain unclear, emerging evidence supports a role for Pdx-1 as a key transcription factor for specific gut endocrine cell lineages. Introduction of pdx-1 into rat IEC-6 intestinal epithelial cells induced differentiation into an enteroendocrine phenotype, with induction of chromogranin A, serotonin, CCK, gastrin and somatostatin. See Differentiation of immature enterocytes into enteroendocrine cells by Pdx1 overexpression Am. J. Physiol. 2001;281 229-236
Several genes appear important for both islet and endocrine cell development. For example, mice with the SEYNEU mutation exhibit defective islet organization and markedly reduced numbers of glucagon- immunopositive L cells as described in Mol Endocrinol 1999 Sep;13(9):1474-86 Essential requirement for Pax6 in control of enteroendocrine proglucagon gene transcription
Similarly, the Notch signaling pathway appears essential for the regulation of islet and enteroendocrine cell development, see Nat Genet 2000 Jan;24(1):36-44 Control of endodermal endocrine development by Hes-1. Impairment of NOTCH signaling increases the numbers of secretory cells within the gut epithelium and Ngn3 expression in progenitors directs these cells towards and enteroendocrine lineage. Indeed, Petersen et al used the NOTCH signaling pathway gamma secretase inhibitor dibenzazepine to increase the number of murine and human L cells in respective organoid cultures. Treatment of HFD mice with dibenzazepine also increased the number of functional L cells, enhanced GLP-1 and insulin secretion and lowered blood glucose, actions blocked by the GLP-1R antagonist exendin(9-39). These experiments provide proof of concept for efforts directed at increasing L cell number. Targeting development of incretin-producing cells increases insulin secretion J Clin Invest. 2014 Dec 15. pii: 75838. doi: 10.1172/JCI75838
The neurogenin gene is important not only for the formation of islet cell lineages, but also determines specification of gastric endocrine cell lineages in the mouse, including glucagon-immunopositive gastric endocrine cells, as shown in Neurogenin 3 is essential for the proper specification of gastric enteroendocrine cells and the maintenance of gastric epithelial cell identity. Genes Dev. 2002 Jun 15;16(12):1488-97 Similarly, disruption of Ngn-3 produces abnormalities in multiple intestinal endocrine cell lineages as shown in Neurogenin3 is differentially required for endocrine cell fate specification in the intestinal and gastric epithelium. EMBO J. 2002 Dec 2;21(23):6338-47. Conditional deletion of ngn-3 in the gut using the villin-Cre mouse in the CD1 background resulted in the ablation of numerous enteroendocrine cell lineages. These mice died with a very high frequency during the first week of life. Surviving mice exhibited numerous abnormalities including fat malabsorption, watery stools, reduced weight gain, reduced body fat, improved insulin sensitivity and glucose tolerance, increased gut transit, increased crypt cell proliferation, increased cell turnover, abnormal architecture in the villus and crypt compartment and shorter microvilli, abnormal allocation of islet cell lineages and abnormalities in islet size. The interpretation of this phenotype is complicated due to the profound weight loss and simultaneous deficiency of multiple peptide hormones. Loss of enteroendocrine cells in mice alters lipid absorption and glucose homeostasis and impairs postnatal survival. J Clin Invest. 2010 May 3;120(5):1708-21.
The transcription factor Arx is expressed in developing murine and human enteroendocrine cell populations, in subsets of cells + for Pdx1, Ngn3 and isl-1. Genetic removal of Arx from the gut endoderm using Foxa3-Cre mice resulted in growth retardation, diarrhea, and reduced numbers of gastrin- and glucagon-producing cells in the stomach, with a marked reduction of CCK, glucagon, and GLP-1+ cells in the mouse duodenum, jejunum, and ileum. Deletion of Arx from the epithelial compartment using Villin-Cre mice resulted in chronic diarrhea, and reduced numbers of CCK+ and GLP-1+ cells in the duodenum. Knockdown of Arx in ES cell derived human intestinal organoids reduced CCK, secretin and proglucagon gene expression. Arx is required for normal enteroendocrine cell development in mice and humans Dev Biol. 2012 Feb 24.
The Drucker lab has isolated and studied a mouse enteroendocrine cell line, designated GLUTag. GLUTag cells respond to the same secretagogues that normally regulate rat enteroendocrine cell function, and appear highly differentiated when compared to the behavior of normal rat intestinal endocrine cells. For a direct comparison of FRIC cultures and GLUTag cells, see Endocrinology 1998 Oct;139(10):4108-14 Regulation of glucagon-like peptide-1 synthesis and secretion in the GLUTag enteroendocrine cell line . L cells appear to be glucose-sensitive and contain multiple ion channels, glucose transporters and glucokinase Glucose-sensing in glucagon-like peptide-1-secreting cells Diabetes. 2002 Sep;51(9):2757-63. Nevertheless, GLP-1 secretion appears normal in human subjects with glucokinase mutations, hence this molecule is unlikely to be essential for glucose-stimulated GLP-1 secretion in L cells Glucokinase, the pancreatic glucose sensor, is not the gut glucose sensor. Diabetologia. 2009 Jan;52(1):154-9.
For a more detailed overview of the properties of GLUTag cells, see GLUTag
A comprehensive single cell transcriptomics approach was applied to interrogate enteroendocrine cell lineages at various stages of their development using a combination of mouse epithelium, mouse organoids, and knockdown approaches. The positional heterogeneity, plasticity, importance of positional location, and migration kinetics, was examined for multiple EECs, yielding a large library of information, largely focused on the importance of transcription factors at various strages of differentiation and lineage committment Identification of Enteroendocrine Regulators by Real-Time Single-Cell Differentiation Mapping https://www.cell.com/cell/fulltext/S0092-8674(18)31643-X
A major challenge in the study of the factors that stimulate GLP-1/GLP-2 secretion remains the difficulty in isolating large numbers of viable non-transformed L cells. Gribble and colleagues used a transgenic approach to isolate non-transformed L cells using a fluorescent protein expressed in L cells under the control of the proglucagon promoter. Isolated sorted GLP-1-secreting L cells were analyzed in primary culture. These cells were directly glucose-responsive, and secreted GLP-1 in response to agents causing membrane depolarization or neurotransmitter-stimulated signal transduction. Moreover, comparison of key genes and proteins expressed in and signal transduction pathways operative in L cells with the same genes, proteins, and pathways utilized by the GLUTag cell line revealed remarkable similarities between non-immortalized L cells and GLUTag cells. See Glucose sensing in L cells: a primary cell study Cell Metab. 2008 Dec;8(6):532-9. Follow-up studies compared glucose sensing in isolated purified L cells, Sglt1-/- L cells, and GLUTag cells. Glucose uptake into L cells was found to occur via GLUT transporters. Glucokinase activation potentiated GLP-1 secretion from GLUTag cells but not from primary murine L cells. Inhibition of SGLT activity with phloridzin markedly reduced glucose-stimulated GLP-1 secretion and Sglt1 knockdown in GLUTag cells abolished the stimualtory effects of glucose and alpha-methyl glucose, whereas Sglt1-/- L cells were not responsive to glucose. Predominant role of active versus facilitative glucose transport for glucagon-like peptide-1 secretion Diabetologia. 2012 May 26.
Friedlander and colleagues studied the importance of cAMP, adenylate cyclase, and phsophodiesterase (PDE) using primary murine colonic L cells and GLUTag cells. L cells expressed high levels of adenylate cyclase isoforms 2, 5, 6, 8, and 9. AC2 was preferentially expressed in L cells. Multiple PDE isoforms were also expressed in L cells. Activation of cyclic GMP also stimulated GLP-1 secretion, with PDE3 likely important for these effects. See Role of phosphodiesterase and adenylate cyclase isozymes in murine colonic glucagon like peptide 1 secreting cells Br J Pharmacol. 2010 Nov 3. doi: 10.1111/j.1476-5381.2010.01107.
Rogers et al demonstrated that primary colonic L cells exhibit electrical activity blocked by TTX, consistent with the presence of V-gated Na+ currents and transcriptome analysis demonstrated the presence of multiple Scn alpha and beta subunits. GLP-1 secretion was clearly voltage-dependent, inhibited by diazoxide, and triggered by KCl. Basal and stimulation of GLP-1 secretion by glutamine was partially inhibited by TTX, affirming the importance of Na+ channel activity in GLP-1 secretion. Calcium channel subunits were also expressed in L cells and GLUTag cells and both basal and glutamine-stimulated GLP-1 secretion was inhibited by nifedipine, and w-conotoxin, consistent with a functional role for Q-type currents. See Electrical activity-triggered Glucagon-Like Peptide-1 secretion from primary murine L-cells J Physiol. 2011 Jan 4.
A human intestinal cell line derived from an adenocarcinoma has been characterized in some detail and exhibits endocrine properties, including chromogranin and proglucagon expression. NCI-H716 cells secrete GLP-1 in response to a number of neurotransmitters, nutrients and secretagogues, as described in A human cellular model for studying the regulation of glucagon-like peptide-1 secretion. Endocrinology. 2001 Oct;142(10):4522-8. Nevertheless, the control of proglucagon gene expression and gene transcription is highly aberrant in NCI-H716 and does not at all recapitulate regulation of gene expression inferred from studies of primary intestinal cell cultures. Hence, the utility of these cells as a differentiated experimental model for the human gut L cell lineage is questionable, as outlined in Aberrant Regulation of Human Intestinal Proglucagon Gene Expression in the NCI-H716 Cell Line. Endocrinology. 2003 May;144(5):2025-33
The molecular mechanisms linking fatty acids to GLP-1 secretion from gut endocrine cells remain incompletely understood. Hirasawa and colleagues have identified a GPCR, designated GPR120 that serves as a receptor for fatty acids on gut endocrine cells. Fatty acids activate the receptor in vitro in association with stimulation of GLP-1 secretion. Whether GPR120 is essential for fatty acid-stimulated GLP-1 secretion in vivo remains unclear. See Free fatty acids regulate gut incretin glucagon-like peptide-1 secretion through GPR120. Nat Med. 2005 Jan;11(1):90-4. Epub 2004 Dec 26
A role for PKCz in the oleic acid-induced stimulation of GLP-1 secretion has been described in studies using gut endocrine cells. Reduction of PKCz expression in GLUTag cells, or addition of a PKCz inhibitor significantly diminished the secretory response to oleic acid, as shown in Protein kinase C{zeta} is required for oleic acid-induced secretion of glucagon-like peptide-1 by intestinal endocrine L cells. Endocrinology. 2006 Nov 16;in press
Similar studies using the STC-1 cell line have identified a receptor for bile acids, designated TGR5 (also known as BG37) which is coupled to stimulation of GLP-1 secretion in a cAMP-dependent manner, as described in Bile acids promote glucagon-like peptide-1 secretion through TGR5 in a murine enteroendocrine cell line STC-1. Biochem Biophys Res Commun. 2005 Apr 1;329(1):386-390
GPR119 was originally described as an orphan G protein coupled receptor expressed on islet β-cells, as outlined in Deorphanization of a G protein-coupled receptor for oleoylethanolamide and its use in the discovery of small-molecule hypophagic agents Cell Metab. 2006 Mar;3(3):167-75. Subsequent studies demonstrated that GPR119 was also directly expressed in human and rodent gut endocrine cells, and in GLUTag cells.
The glucoregulatory actions of GPR119 may include a direct role for activation of the receptor in β-cells leading to direct stimulation of insulin secretion. Indeed, GPR119 agonists activate cyclic formation and may enhance insulin secretion from b-cells and b-cell lines Lysophosphatidylcholine enhances glucose-dependent insulin secretion via an orphan G-protein-coupled receptor Biochem Biophys Res Commun. 2005 Jan 28;326(4):744-51. Erratum in: Biochem Biophys Res Commun. 2005 Apr 1;329(1):417 and A role for beta-cell-expressed G protein-coupled receptor 119 in glycemic control by enhancing glucose-dependent insulin release Endocrinology. 2007 Jun;148(6):2601-9. Epub 2007 Feb 8. Erratum in: Endocrinology. 2007 Oct;148(10):4753. However, the observation that GPR119 is also expressed in gut endocrine cells, and in enteroendocrine cell lines such as GLUTag cells, suggests that activation of GPR119 signaling in enteroendocrine cells may lead to increased secretion of gut hormones such as GIP and GLP-1 as demonstrated by Chu and colleagues A Role for Intestinal Endocrine Cell-Expressed GPR119 in Glycemic Control by Enhancing GLP-1 and GIP Release Endocrinology. 2008 May;149(5):2038-47. Although GPR 119 agonists stimulate the secretion of both GLP-1 and GIP in mice, the actions on GIP secretion may be indirect, as GPR119 receptors have not yet been detected on GIP+ gut enteroendocrine K cells. The identity of the endogenous physiological ligand for GPR119 remains uncertain, but one candidate is oleoylethanolamide (OEA). Administration of OEA enhances GLP-1 secretion from GLUTag cells in a PKA-and GPR119-dependent dependent manner and enteral administration of OEA in the rat small bowel increased GLP-1 and insulin secretion in a glucose-dependent manner as outlined in GPR119 is essential for oleoylethanolamide-induced glucagon-like peptide-1 secretion from the intestinal enteroendocrine L-cell Diabetes. 2009 Feb 10. [Epub ahead of print]
Consistent with the importance of GPR119 in the gut endocrine cell, GPR119 agonists appear to preferentially stimulate insulin secretion and lower blood glucose following enteral administration. Accordingly, GPR119 agonists may exert their glucoregulatory actions at least in part indirectly via stimulation of GIP and GLP-1 secretion, which in turn, promote glucose-dependent insulin secretion. Moreover, at least part of the glucoregulatory actions of GPR119 agonists are diminished by co-administration of the GLP-1R antagonist, exendin (9-39), as shown in A Role for Intestinal Endocrine Cell-Expressed GPR119 in Glycemic Control by Enhancing GLP-1 and GIP Release Endocrinology. 2008 Jan 17; [Epub ahead of print]. The functional properties of different synthetic GPR119 agonists, as well as the naturally ocurring molecules, have been characterized in studies of signal transduction and insulin secretion in Endogenous and synthetic agonists of GPR119 differ in signalling pathways and their effects on insulin secretion in MIN6c4 insulinoma cells. Br J Pharmacol. 2008 Aug 25. [Epub ahead of print]
Flock and colleagues studiedthe consequences of GPR119 activation for gut hormone secretion, glucose tolerance, insulin secretion in vivo and in vitro, and gastric emptying in WT and incretin receptor knockout mice. GPR119 activation improved oral glucose tolerance in single incretin receptor knockout mice, but was not sufficient for reduction of glycemic excursion in DIRKO mice. GPR119 activation produced robust increases in GLP-1, GIP and insulin levels in WT and knockout mice. Oral glucose wqs required for optimal glucoregulatory actions of GPR119 as no significant improvement in IP glucose tolerance waqs detected following GPR119 activation, and no improvement in insulin sensitivity was observed. AR231453 directly increased insulin secretion from WT and incretin receptor knockout islets in vitro. The GPR119 agonist AR231453 inhibited gastric emptying in WT, Glp1r-/-, DIRKO, and Glp2r-/- mice and in WT mice treated with a Y2R inhibitor. See
GPR119 Regulates Murine Glucose Homeostasis Through Incretin Receptor-Dependent and Independent Mechanisms
Endocrinology published November 10, 2010 doi:10.1210/en.2010-1047
Although limited information is available about the role of GPR119 in the control of human GLP-1 and/or insulin secretion, a preliminary report by press release describes glucose-lowering properties of a GPR119 agonist designated APD668, in single dose and 14 day administration studies of human subjects, as outlined in the Jan 7 2008 Press Release
Flock and colleagues also identified robust expression of the classical progsterone receptor in GLUTag cells and showed that enteral progesterone stimulates GLP-1 secretion and lowers blood glucose in mice. Remarkably, membrane restricted ligands such as BSA-progesterone also stimulated GLP-1 secretion from GLUTag cells, and inhibition of classical PR signaling with RU486 had no effect on progestin-stimulated GLP-1 secretion and did not impair the ability of progesterone to improve glucose homeostasis in vivo. GLUTag cells also expressed membrane progesterone receptors Paqr5 and Paqr7, and knockdown of these receptors in GLUTag cells eliminated the progestin-dependent stimulation of GLP-1 secretion. Nevertheless, enteral progesterone was still capable of increasing insulin and lower glucose even in mice with disruption of both the Glp1r and Gipr. These findings raise the possibility that gut restricted membrane progestrone receptor agonists may be capable of enhancing incretin secretion and lowring glucose in vivo. Activation of Enteroendocrine Membrane Progesterone Receptors Promotes Incretin Secretion and Improves Glucose Tolerance in Mice Diabetes. 2012 Aug 29.
The related GPCR designated GPR40 may also play a role in the control of murine gut hormone secretion. GPR40 was localized to subsets of GIP and GLP-1+ endocrine cells in the murine gut and GPR4-/- mice exhibit defective incretin secretion in response to acute administration of fat, whereas GIP and GLP-1 secretion is normal in GPR40-/- mice See Gpr40 is expressed in enteroendocrine cells and mediates FFA stimulation of incretin secretion. Diabetes. 2008 Jun 2. [Epub ahead of print]
Genetic ablation of L cells in mice was achieved through selective targeting of Diphtheria Toxin using the proglucagon promoter to targetenteroendocrine L cells. Mice with depletion of L cells exhibited enhanced intestinal mucosal damage to cytotoxic chemical injury, phenotypes rescued by combined administration of GLP-1 and GLP-2 agonists. Endogenous glucagon-like peptide- 1 and 2 are essential for regeneration after acute intestinal injury in mice PLoS One. 2018 Jun 4;13(6):e0198046
Where does GLP-1 come from? The islets vs. the gut?
Despite the preponderance of evidence demonstrating the synthesis and secretion of bioactive GLP-1 in the small and large intestine studies have also implicated pancreatic islet a-cells as a source of bioactive GLP-1. Rodent and human islet cells cultured ex vivo secrete GLP-1 with insulinotropic activity. Moreover, experimental pancreatic injury, including surgical manipulation, chemical damage, aging, or the prolonged nutritional stress of energy dense diets, is associated with increased pancreatic production of GLP-1, as reviewed in Incretin Action in the Pancreas: Potential Promise, Possible Perils, and Pathological Pitfalls Diabetes. 2013 Oct;62(10):3316-23.
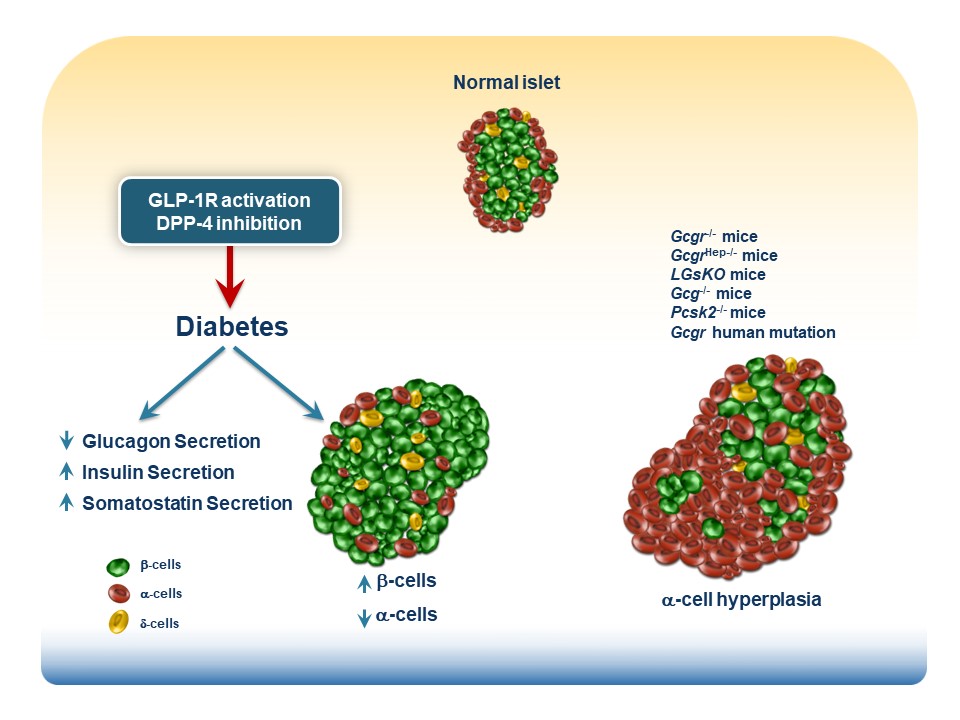
Studies by Chambers, Sandoval and colleagues used mouse genetics and the GLP-1R antagonist exendin(9-39) to examine the consequences of selective re-induction of endogenous Gcg gene expression in the intestine vs. the pancreas of Gcg-/- mice. Reactivation of intestinal Gcg expression using the Villin-Cre system (GcgRA?VilCre) restored intestinal Gcg and GLP-1 production, in the setting of complete loss of pancreatic Gcg expression. Surprisingly, the GLP-1R antagonist exendin(9-39) failed to impair glycemic excursions to both oral and intraperitoneal (i.p.) glucose loads in GcgRA?VilCre mice. In contrast, selective reactivation of pancreatic Gcg expression in GcgRA?PDX1Cre mice and concomitant administration of exendin(9-39) led to impairment of glycemic excursions in both oral and i.p. glucose tolerance tests. Collectively, these observations elevated the putative importance of the pancreas as a key source for GLP-1 action The Role of Pancreatic Preproglucagon in Glucose Homeostasis in Mice Cell Metab. 2017 Apr 4;25(4):927-934.e3
Interpretation of these findingsrequires careful consideration of the experimental context, namely reactivation of Gcg expression inGcg-/- mice known to exhibit alpha-cell hyperplasia. These conditions favor generation of pancreatic islet GLP-1 production in dedifferentiated alpha-cells following reintroduction of pancreatic Gcg expression. Moreover, Gcg-/- mice may exhibit compensatory induction of islet beta-cell GIP expression Ectopic Expression of GIP in Pancreatic β-Cells Maintains Enhanced Insulin Secretion in Mice With Complete Absence of Proglucagon-Derived Peptides Diabetes. 2013 Feb;62(2):510-8 further complicating interpretation of incretin action. Critically, the importance of pancreatic vs. intestinal GLP-1 activity was inferred indirectly via the glycemic response to exendin(9-39) The Role of Pancreatic Preproglucagon in Glucose Homeostasis in Mice Cell Metab. 2017 Apr 4;25(4):927-934.e3. Since the publication of these provocative findings, several studies have demonstrated that exendin(9-39) also blocks the insulinotropic actions of glucagon at the islet GLP-1 receptor β Cell Tone Is Defined by Proglucagon Peptides Through cAMP Signaling JCI Insight. 2019 Mar 7;4(5):e126742 and Insulin Secretion Depends on Intra-islet Glucagon Signaling Cell Rep. 2018 Oct 30;25(5):1127-1134 and Intra-islet Glucagon Signaling Is Critical for Maintaining Glucose Homeostasis JCI Insight. 2019 Apr 23;5(10):e127994 complicating precise mechanistic attribution of glycemic responses following use of exendin(9-39).
To better understand the relative role of the proximal vs. the distal gut in the generation of circulating GLP-1, Youngmi Song and Jackie Koehler generated lines of mice with substantial elimination of Gcg expression in both the small and large intestine (GcgGut-/-) or more selective loss of distal gut Gcg expression in the terminal ileum and colon (GcgDistalGut-/-). Analysis of these mice reinforced the importance of the gut as the predominant source of circulating GLP-1. Proglucagon-Derived Peptides Are Essential for Regulating Glucose Homeostasis in Mice Cell Metab. 2019 Nov 5;30(5):976-986.e3 Unexpectedly, circulating levels of GLP-1 were also lower in the fasting state, and glucose tolerance was impaired in GcgDistalGut-/- mice, prompting ongoing questions about the relative contributions of the proximal vs. distal gut to the control ofGLP-1levels in the interprandial state and following nutrient ingestion. Brandon Panaro queried the importance of the proximal vs. the distal gut for the acute response to GLP-1 secretagogues. Olive oil, arginine and glucose increase GLP-1 levels in the circulation without requiring contributions from the distal gut. However LPS, GPR119 agonists, and metformin require distal gut Gcg expression for a robust increase in plasma GLP-1 expression. See Intestine-selective Reduction of Gcg Expression Reveals the Importance of the Distal Gut for GLP-1 Secretion Mol Metab. 2020 Apr 9;37:100990
A video describing the Panaro Mol Metabolism paper is here
Are there examples of enteroendocrine cell deficiency in human disease states? Although admittedly rare, patients with autoimmune polyglandular endocrine failure may exhibit a deficiency of gut endocrine cells, leading to clinical disease. For example, review the case report describing a marked reduction in the number of CCK+ enteroendocrine cells in a human patient with fat malabsorption and diarrhea in the NEJM; Malabsorption due to cholecystokinin deficiency in a patient with autoimmune polyglandular syndrome type I. N Engl J Med. 2001 Jan 25;344(4):270-4.
Although the principal function of enteroendocrine cells is classically to synthesize and secrete gut hormones, enteroendocrine cells may also express TLRs which are important for innate immunity in response to environmental challenge. The TLR ligands LPS, flagellin, or CpG oligonucleotides activate their cognate TLRs on STC-1 cells and enhance L cell secretion leading to release of gut hormones, chemokines and b-defensin-2 both in vitro and in vivo, as described in Activation of Enteroendocrine Cells via TLRs Induces Hormone, Chemokine, and Defensin Secretion. J Immunol. 2007 Apr 1;178(7):4296-303.
Are there examples of enteroendocrine cell hyperfunction leading too increased circulating levels of gut peptides that contribute to the development of syndromes in human subjects? See Gut hormones and Bariatric Surgery for an overview
